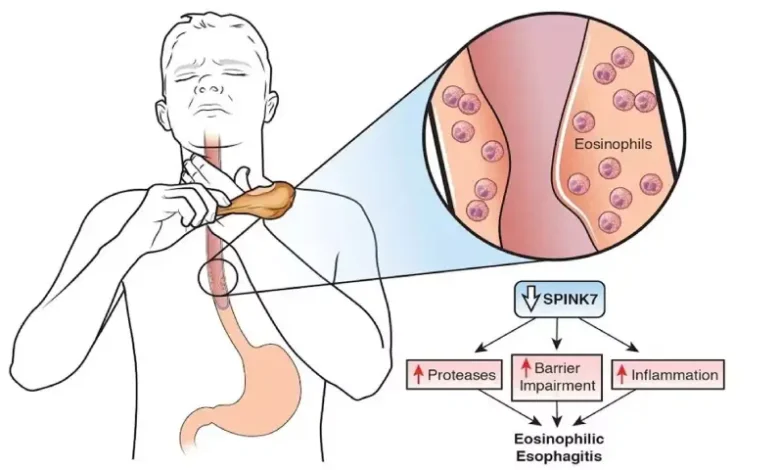
Eosinophilic oesophagitis is a chronic inflammatory condition affecting the oesophagus, the tube that carries food from the mouth to the stomach. In the context of eosinophilic esophagitis NHS UK services, it is increasingly recognised as an important digestive disorder that requires specialist diagnosis and long-term management. It develops when eosinophils, a type of white blood cell, build up in the oesophagus and trigger inflammation, swelling, and difficulty swallowing.
Within eosinophilic esophagitis NHS care pathways, the condition is often first mistaken for acid reflux or food intolerance due to overlapping symptoms. However, growing awareness across NHS gastroenterology departments has improved diagnostic accuracy. Although it is not usually life-threatening, eosinophilic esophagitis NHS UK management is essential because untreated inflammation can lead to narrowing of the oesophagus and ongoing swallowing difficulties.
Causes and risk factors of eosinophilic oesophagitis
The exact cause of eosinophilic oesophagitis remains complex, but it is widely linked to abnormal immune responses to certain foods or environmental triggers. In eosinophilic esophagitis NHS evaluations, food allergens such as dairy, wheat, eggs, soy, nuts, and seafood are frequently identified as contributing factors. These triggers can cause persistent inflammation in susceptible individuals.
Research within eosinophilic esophagitis NHS UK settings also highlights a strong association with allergic conditions. People who suffer from asthma, eczema, or hay fever are more likely to develop this condition. Genetic predisposition and immune system sensitivity play an important role, making it a condition that often appears alongside other allergic disorders in both children and adults.
Symptoms of eosinophilic oesophagitis
One of the most common symptoms seen in eosinophilic esophagitis NHS patients is difficulty swallowing, medically known as dysphagia. Food may feel stuck in the throat or chest, leading to discomfort, slow eating, and anxiety during meals. Over time, this symptom may worsen, especially if inflammation continues without treatment.
Other symptoms associated with eosinophilic esophagitis NHS UK cases include chest pain, heartburn-like sensations, regurgitation, and food avoidance. In children, symptoms may present differently, including poor appetite, vomiting, or failure to thrive. These symptoms are often mistaken for common digestive problems, which is why early NHS assessment is essential for accurate diagnosis.
Diagnosis of eosinophilic oesophagitis in the NHS UK
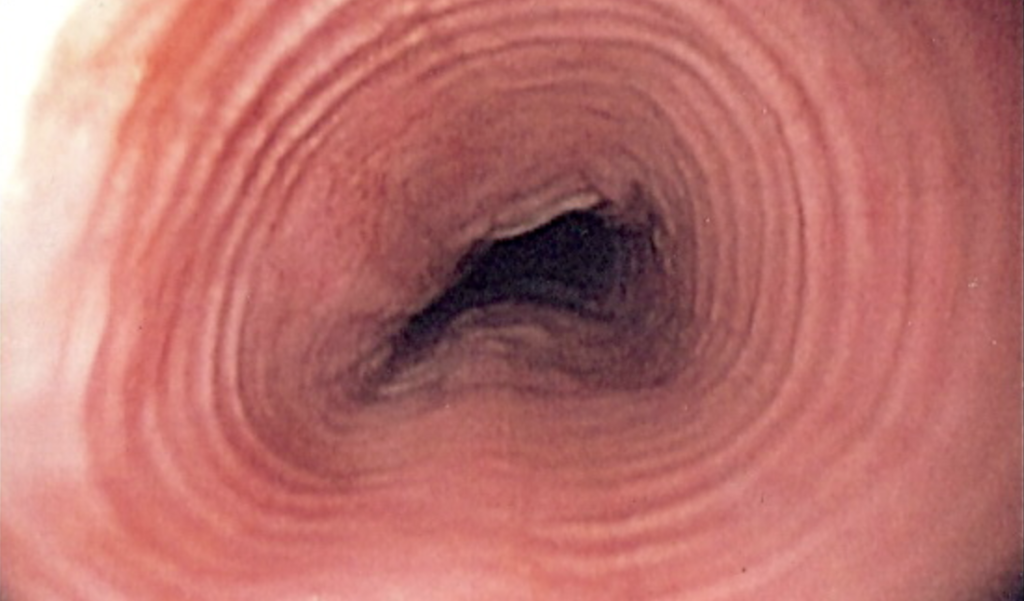
Diagnosis of eosinophilic esophagitis NHS cases typically involves referral to a gastroenterologist. The main diagnostic procedure is an endoscopy, where a thin tube with a camera is inserted into the oesophagus to visually inspect the lining. During this process, small tissue samples or biopsies are taken to detect eosinophil levels.
In eosinophilic esophagitis NHS UK diagnostic pathways, biopsy results are crucial for confirmation. Doctors also rule out other conditions such as gastroesophageal reflux disease (GERD), infections, or structural abnormalities. Although allergy testing may be carried out, it is not always definitive. A combination of clinical symptoms, endoscopic findings, and biopsy results is required for a confirmed diagnosis.
Treatment options for eosinophilic oesophagitis
Treatment for eosinophilic esophagitis NHS patients focuses on reducing inflammation and improving swallowing function. One of the most common first-line treatments is proton pump inhibitors, which help reduce acid and inflammation in the oesophagus. These medications can significantly improve symptoms in many patients.
In eosinophilic esophagitis NHS UK treatment plans, swallowed topical steroids such as budesonide or fluticasone are often used when symptoms persist. These medications target inflammation directly in the oesophagus. In addition, doctors may recommend oesophageal dilation in cases where narrowing has occurred, helping restore normal food passage.
Dietary management and elimination diets
Diet plays a crucial role in eosinophilic esophagitis NHS management. Many patients benefit from elimination diets, where common trigger foods are removed under the supervision of a dietitian. This approach helps identify specific allergens responsible for inflammation and allows for more personalised long-term dietary control.
Within eosinophilic esophagitis NHS UK care, elimination diets often start with removing major triggers such as dairy and wheat, followed by gradual reintroduction. Although challenging, this method can significantly reduce symptoms and improve quality of life. NHS dietitians play an important role in ensuring nutritional balance is maintained throughout the process.
Living with eosinophilic oesophagitis
Living with eosinophilic esophagitis NHS care requires ongoing management and lifestyle adjustments. As a chronic condition, it does not typically go away completely, but symptoms can be controlled effectively with the right treatment plan. Regular follow-ups with NHS specialists are essential for monitoring progress and adjusting therapies when needed.
Patients living with eosinophilic esophagitis NHS UK often adapt their eating habits to reduce discomfort. Eating slowly, chewing thoroughly, and avoiding known trigger foods can make a significant difference. Emotional support is also important, as anxiety around eating and social situations can affect overall wellbeing and confidence.
Complications of untreated eosinophilic oesophagitis
If eosinophilic esophagitis NHS cases are left untreated, inflammation can lead to serious complications. One of the most common is oesophageal narrowing, also known as strictures, which makes swallowing increasingly difficult. This condition may require medical procedures such as dilation to restore normal function.
In eosinophilic esophagitis NHS UK patients, untreated disease can also lead to food impaction, where food becomes stuck in the oesophagus and requires emergency removal. Chronic inflammation may further reduce quality of life and increase nutritional deficiencies, highlighting the importance of early diagnosis and consistent treatment.
When to seek urgent NHS care
Recognising when to seek urgent care is essential in eosinophilic esophagitis NHS management. If food becomes stuck in the throat or chest and does not pass naturally, immediate medical attention is required. This condition, known as food bolus obstruction, can become a medical emergency.
In eosinophilic esophagitis NHS UK guidelines, patients are advised to attend A&E if they experience severe chest pain, inability to swallow saliva, or persistent obstruction. Early intervention helps prevent complications and ensures safe removal of the blockage, reducing the risk of further oesophageal damage.
Conclusion
Eosinophilic esophagitis NHS UK care focuses on long-term management rather than a permanent cure. With early diagnosis, appropriate medication, and dietary adjustments, most patients can achieve significant symptom control. Awareness of eosinophilic esophagitis NHS pathways continues to improve across the UK, leading to better outcomes for patients of all ages.
Understanding eosinophilic esophagitis NHS treatment options and lifestyle changes is key to managing this chronic condition effectively. With ongoing NHS support, specialist guidance, and patient awareness, individuals can lead a comfortable life while keeping symptoms under control and preventing complications.





